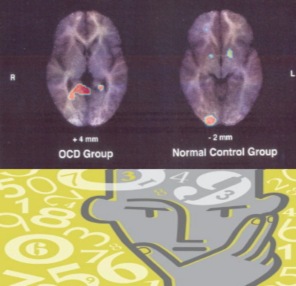
Obsessive–compulsive disorder
Obsessive–compulsive disorder (OCD) is an anxiety disorder characterized by involuntary intrusive thoughts. When a sufferer begins to acknowledge these intrusive thoughts, the sufferer then develops anxiety based on the dread that something bad will happen. The sufferer feels compelled to voluntarily perform irrational, time-consuming physical behaviors to diminish the anxiety.
Sufferers often try to keep their compulsive behaviors hidden from others, often to avoid embarrassment, humiliation or to avoid being seen as strikingly odd or different from others. If the condition is not realized by an undiagnosed sufferer, they may scold themselves in frustration as to why they are thinking or acting the way they are. Although the acts of those who have OCD may appear paranoid and come across to others as psychotic, an OCD sufferer is able to recognize their thoughts and subsequent actions as irrational, which is what makes the illness so distressing. The psychological self-awareness of the irrationality of the disorder may be painful; a sufferer may be plagued by doubt and uncertainty regarding their own feelings and behaviors. A principal challenge faced by OCD sufferers is learning to manage their own behaviors without constant reassurance from others.
OCD is the fourth most common mental disorder and is diagnosed nearly as often as the physiological ailments asthma and diabetes mellitus. In the United States, one in 50 adults has OCD. The phrase "obsessive–compulsive" has become part of the English lexicon, and is often used in an informal or caricatured manner to describe someone who is meticulous, perfectionistic, absorbed in a cause, or otherwise fixated on something or someone. Although these signs are often present in OCD, a person who exhibits them does not necessarily have OCD, and may instead have obsessive–compulsive personality disorder (OCPD) or some other condition.
DSM IV Obsessive Compulsive Disorder (OCD) Criteria
A. Either obsessions or compulsions:
Obsessions as defined by (1), (2), (3), and (4):
(1) recurrent and persistent thoughts, impulses, or images that are experienced at some time during the disturbance, as intrusive and inappropriate and that cause marked anxiety or distress
(2) the thoughts, impulses, or images are not simply excessive worries about real-life problems
(3) the person attempts to ignore or suppress such thoughts, impulses, or images, or to neutralize them with some other thought or action
(4) the person recognizes that the obsessional thoughts, impulses, or images are a product of his or her own mind (not imposed from without as in thought insertion)
Compulsions as defined by (1) and (2):
(1) repetitive behaviors (e.g., hand washing, ordering, checking) or mental acts (e.g., praying, counting, repeating words silently) that the person feels driven to perform in response to an obsession, or according to rules that must be applied rigidly
(2) the behaviors or mental acts are aimed at preventing or reducing distress or preventing some dreaded event or situation; however, these behaviors or mental acts either are not connected in a realistic way with what they are designed to neutralize or prevent or are clearly excessive
B. At some point during the course of the disorder, the person has recognized that the obsessions or compulsions are excessive or unreasonable. Note: This does not apply to children.
C. The obsessions or compulsions cause marked distress, are time consuming (take more than 1 hour a day), or significantly interfere with the person’s normal routine, occupational (or academic) functioning, or usual social activities or relationships.
D. I another Axis I disorder is present, the content of the obsessions or compulsions is not restricted to it (e.g., preoccupation with food in the presence of an Eating Disorder; hair pulling in the presence of Trichotillomania; concern with appearance in the presence of Body Dysmorphic Disorder; preoccupation with drugs in the presence of a Substance Use Disorder; preoccupation with having a serious illness in the presence of Hypochondriasis; preoccupation with sexual urges or fantasies in the presence of a Paraphilia; or guilty ruminations in the presence of Major Depressive Disorder).
E. The disturbance is not due to the direct physiological effects of a substance (e.g., a drug of abuse, a medication) or a general medical condition.

 Brazilian Center of Transcranial Magnetic Stimulation - CBrEMT
Brazilian Center of Transcranial Magnetic Stimulation - CBrEMT